We use it to communicate, nourish our body, and connect with others. Yet it can also unwind the health and behavior of children when misused. Our mouths are an invitation into the body, that when left open and unchecked permit open destruction that is difficult to resolve. I’ve been there with sick and tired children, there are no happy endings if it’s left to be “grown out of”, just more illness, specialists, and medication. Knowing what to look for and what to do can dramatically impact your child’s health, growth, learning and behavior.
“If mouth breathing is treated early, its negative effect on facial
Yosh Jefferson, DMD, MAGD
and dental development and the medical and social problems
associated with it can be reduced or averted”
The mouth is the gateway into the body. For some of the same reasons that we tell our kids not to put dirty fingers or food that fell on the floor in their mouths, we should tell them to keep their mouths closed. The nose filters and humidifies the air we breathe, optimizing every breath. The mouth lacks the same structures and as such leaves the growing child susceptible to various illness, developmental, and behavioral problems.
Often unchecked, as most health care providers are unaware of the negative impact of mouth breathing, the effects are long-term and frequently treated with medication and surgery. Parent to parent, here is everything you need to know about mouth breathing and how to treat it.

Sleep and growth become compromised
Mouth breathing is often accompanied by and a causative factor of upper airway resistance. Enlarged tonsils and adenoids that prevent the quiet flow of air through the nose and airway present as mouth and audible breathing during waking hours. At night, when the muscles relax and the body is horizontal it presents as snoring, restless sleep, abrupt stops in breathing, gasping, and insomnia.
Also known, as sleep-disordered breathing, these airway issues that occur during sleep can negatively impact growth, focus, and behavior. It is nearly impossible to reach stage 3 deep sleep when the body is not properly oxygenating. It takes the body into fight or flight and wakes itself periodically to remain alive. Children who are not reaching deep sleep are losing out on the stage when the growth hormone is secreted and can impact their height, weight, and restoration.

“(C)hildhood obstructive sleep apnea syndrome is a dynamic process resulting from a combination of structural and neuromotor abnormalities, rather than from structural abnormalities alone.”
Carole L. Marcus
Cognitive and behavioral problems occur
Tired children are different from tired adults. Often a tired child will be hyperactive and restless during waking hours as opposed to fatigue an adult will show. Research has shown that misconception of the symptoms of ADHD and sleep-disordered breathing are associated.
Poor sleep, as mentioned above, where the brain is not properly oxygenated due to upper airway resistance can create difficulty with focus, organization, self-regulation of emotions, and poor behavioral control.
“Children whose symptoms peaked early—at 6 or 18 months—were 40 percent and 50 percent more likely, respectively, to experience behavioral problems at age 7 compared with normally-breathing children.”
Dr. Karen Bonuck
Heart and blood pressure problems are more likely
Nasal breathing has the benefit of increasing the nitric oxide in the body and aiding in smooth muscle relaxation. A body fueled on mouth breathing has a lower oxygen concentration, which is associated with high blood pressure and cardiac failure. Though seen more commonly in adult patients, a chronic buildup of poor oxygenation makes a child more likely to experience these problems in their future.
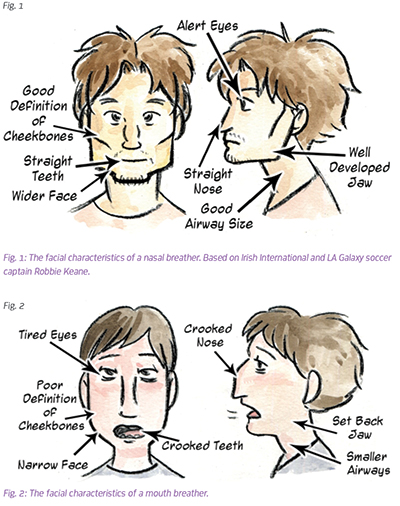
Altered facial appearance and dental malocclusion
Your lips act as your face’s braces and your tongue acts as your palate’s expander. In ideal oral resting posture, the tongue sits up against the roof of the mouth and the constant pressures of that posture develop a wide arch. Mouth breathing with open lips, or low tongue resting posture is the real reason braces come into play.
Narrow dental arches, mean a narrow nasal floor and can cause a deviated septum, adenoid hypertrophy, and pinched nostrils. This narrow development causes a “long face” appearance. Often coupled with allergic shiners or pooling of blood vessels that creates darkness under the eyes.
Poor Posture
Mouth breathing compromises the size of a growing airway. Where there is a problem within the body, the body finds a way to compensate and adjust. The head will tilt forward and up to superficially open the airway to accommodate for the poor oxygenation. This forward head posture is often accompanied by shoulders that are rolled forward, unstable core, and poor posture.
“Changing the mode of breathing from oral to nasal early in adolescence may promote a tendency towards normalization of the craniofacial dimensions with growth.”
Antonio M Cuccio et. al
How to stop your child’s mouth breathing without nagging, stress, or losing your mind
Step 1, know what to look for. Common symptoms include:
- Frequent lip apart mouth posture
- Audible breathing
- Frequent congestion
- Snoring, gasping, or restless sleep
- Allergic shiners
- Poor focus and attention
- Long face appearance
- Narrow dental arches or malocclusion
- Behavioral problems
Or, do one of our definitive assessments.
Step 2, rule out physical barriers.
A thorough exam by a medical specialist, such as an ENT or sleep physician can rule out severe tonsil/adenoid obstruction and/or sleep apnea. The prescense of which would prohibit a conservative and natural approach to resolution.
Step 3, speak to a myofunctional therapist.
Myofunctional therapy, also known as orofacial myology, is the voluntary art of neuromuscular modification and reeducation to enable proper oral resting posture. The attainment of which allows for proper body oxygenation, chewing and swallowing. This process involves engaging in various exercises and activities to establish new muscular patterning.
With a history of evidence-based research to accompany this century-old therapeutic process, it is a time-tested and proven method to achieve nasal breathing. Effective at any age, myofunctional therapy has greater results with children.
“Current literature demonstrates that myofunctional therapy decreases apnea-hypopnea index by approximately 50% in adults and
Dr. Camario Camacho et. al
62% in children”
For more on our dynamic myofunctional therapy program that combines traditional therapy with breath, brain, and body work, for greater impact and faster results; visit our website and schedule your FREE consultation.

thank you so much. My son is 12 now and we have to fix this! It started 2 maybe 3 years ago now since his teeth grew into an overbite
LikeLike