There would be no bigger lie than to state that as a myofunctional therapist I had no worries going into my 9-year-old daughter’s release. I waited for a little over two years from the time I became a therapist and longer since discovering she was tongue tied before we released. Why? Well, I was scared.
I have complete confidence in my cases with many successful results. I know the process and what is required in active wound management. What would cause my hesitation? It’s my baby!
It’s easier to teach and preach, than to do. So I can identify and admit my fault in this, especially after we had not only an exceptional release, but also an outstanding recovery!
I’m ready to share the inside scoop on our journey from release to recovery, and all that I have learned along the way, in hopes of giving other hesitant parents help and hope.

Restricted to Released
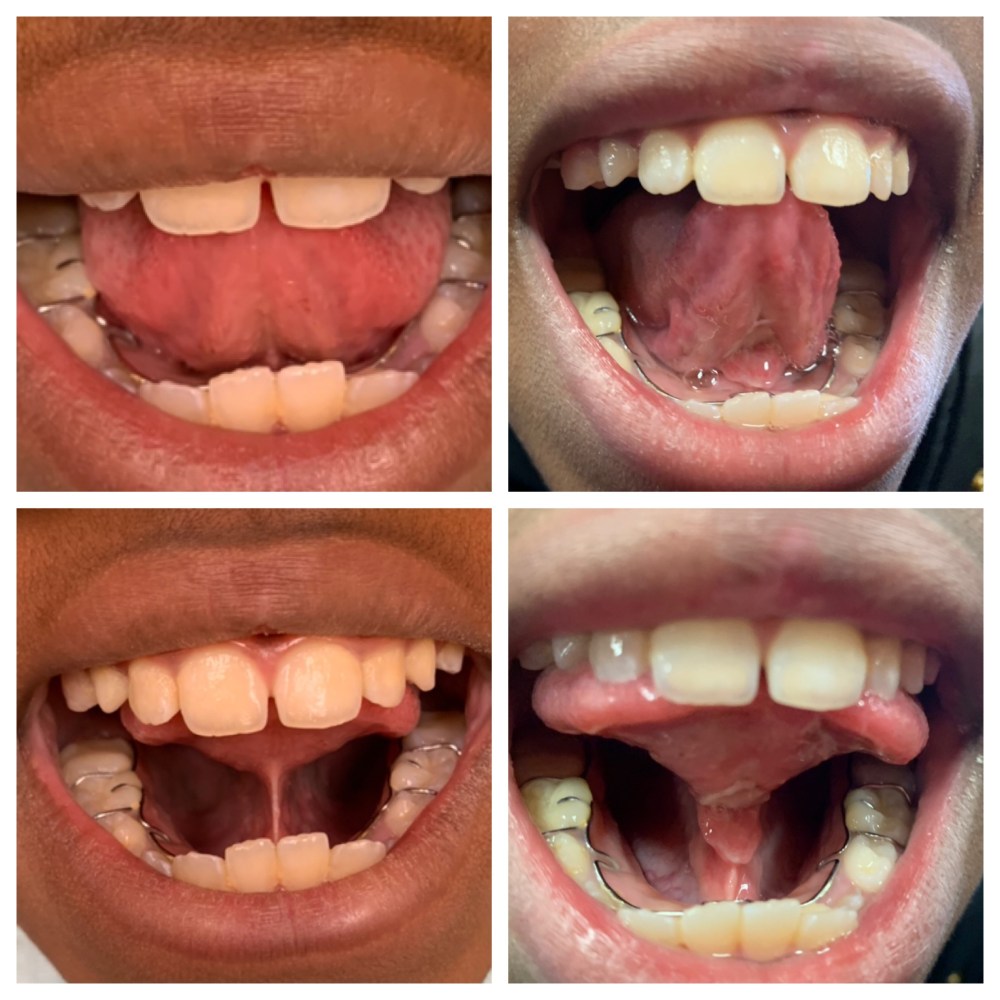
All families should go into a release FULLY prepared. That means you have done your research, interviewed and found an appropriate release provider, and have a recovery plan.
All research should lead you to a myofunctional therapist prior to considering a release. We assess for tongue function and not just appearance. Therapy should begin for a few weeks prior to release as an adjunctive aid in post-release active wound management.
Myofunctional therapy has been an active part of my home for years. My children can cave (a.k.a. suction) and hold on command. There need not be an official time, reason, or purpose, but when asked for any exercise, they perform. Our osteopath asked monthly when we would be doing her release. I knew we needed it, I had everything in place for a long time prior, and preparation was not a problem.
I work daily with a preferred provider, so knew when the time came and I got my feelings in check, she would do the release. My concerns laid solely with my daughter because she is highly sensitive. Tears flow freely and indiscriminately for even the slightest discomfort. Osteopathy and ALF appliance treatment helped with this. However, as a mother it is concerning to think you will put your child in a surgical situation where she will be awake, and then spend days in pain actively managing the wound.
Which leads me to my Pro Tip #1: Ask Questions!
I have assisted during the laser surgical release of babies with this provider. I am keenly aware of what goes down for babies and used that knowledge to inform parents of older children what to expect. While I knew she used local anesthesia for the older children, I had no idea she also used a higher quality topical as a precursor. My daughter sat in the chair with nitrous oxide over her nose enjoying a movie while the injections under the tongue happened. She actually asked at the end if they did the surgery! It was gloriously uneventful and amazingly pleasant.
Ask the provider all the important questions to ease your fears. If you get answers you don’t like, then please contact the office of another provider to ask the questions. Don’t wait in fear, and know what to expect upfront.
Pro tip#2: Stock Up On Cold
Immediately following the procedure we gave her an Italian ice. Exercises needed to be done as soon as possible, and the cold aided in “numbing” the tongue post procedure. The time it takes for the anesthesia to wear off varies based on individual dosage given, absorbed, and processed. Some of my clients are regaining their feeling shortly after the procedure while we are reviewing exercises, and some have 2 hours after leaving before they regain awareness of their tongue. Be prepared for pain management with more than over the counter pain killers, but also with cold relief foods such as yogurt, popsicles, smoothies, refrigerated fruit, ice cream, Italian ice, etc.
Pro tip #3: Wake Up Ready
During my post release protocol, I have my clients move their tongue often for proper healing. I was surprised to find that every morning my daughter’s wound closed overnight. This may be what some would term as “reattachment.” Reattachment will remain in quotes, as there is rarely true reattachment of the frenum. The surgical release is actually a misnomer, as it usually involves excision, or removal, of the frenum tissue. Improper healing usually results in closure of the wound area, and not a connection of the tissue as it was.
As can be seen in the video below, every morning for about a week, we had to re-open the diamond. So we started our mornings with ice and her over the counter NSAID prior to stretching out that tongue to expose the diamond.
Warning! Do not watch the video posted below if you have an aversion to open wounds, blood, or graphic medical images!
Pro tip #4: Little Bleeding, No Biggie
Those who viewed the video above can see that during healing it is possible to see some blood and redness. A few drops of blood, minor bleeding and redness can be very normal, and often should be expected. Have a plain black tea bag ready for any instance of uncomfortable bleeding. Place it under the tongue and rest for 1 minute and then discard. It should eliminate minor bleeding episodes, however, seek medical help or attention for excessive bleeding. Always consult the release provider or your medical physician when concerned.
Pro tip #5: Marathon, Not a Race
Usually, people plan to exercise and stretch for 1-2 weeks post procedure. While I always inform my patients that they will be exercising for 6-8 weeks, I know from experience it is hard to anticipate how long that process is. My daughter had me in the home to instruct her on exercises frequently for 2 weeks, after that, life kicked in and I felt confident that we would relax some. However, these wounds take time to heal completely, so plan on exercising that full 6-8 weeks. We are two months post procedure, and there’s a slight connection that I did not anticipate seeing this late in the game. It’s definitely hard to take your own advice, so heed my warning and plan for the long haul for optimal healing.
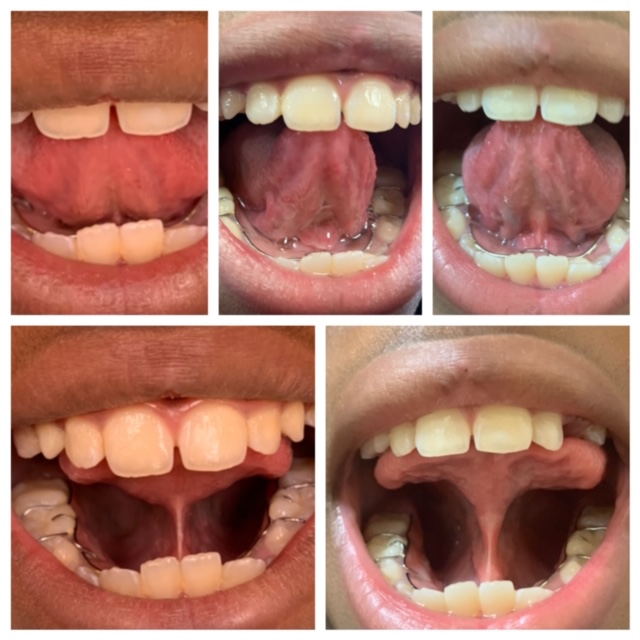
Take Aways
I committed to learning something new during this process, and have actually learned far more than anticipated. It’s a long journey, but if you commit, go in fully informed, stock up on key items and keep that wound open, you will have a successful post release experience.
Click to read more on lip ties, tongue ties, and baby ties

One thought on “Tongue Tie Release Terrors and Triumphs: Releasing the Child of A Myofunctional Therapist”